Shock Wave Therapy: A Non-Invasive Stem Cell Regenerative Technology
For the past 2 years, I've been researching and studying modern applications in regenerative medicine and technology.
The idea of stimulating the body's own ability to heal, and regenerate, is fascinating and very much in line with my personal philosophy on health.
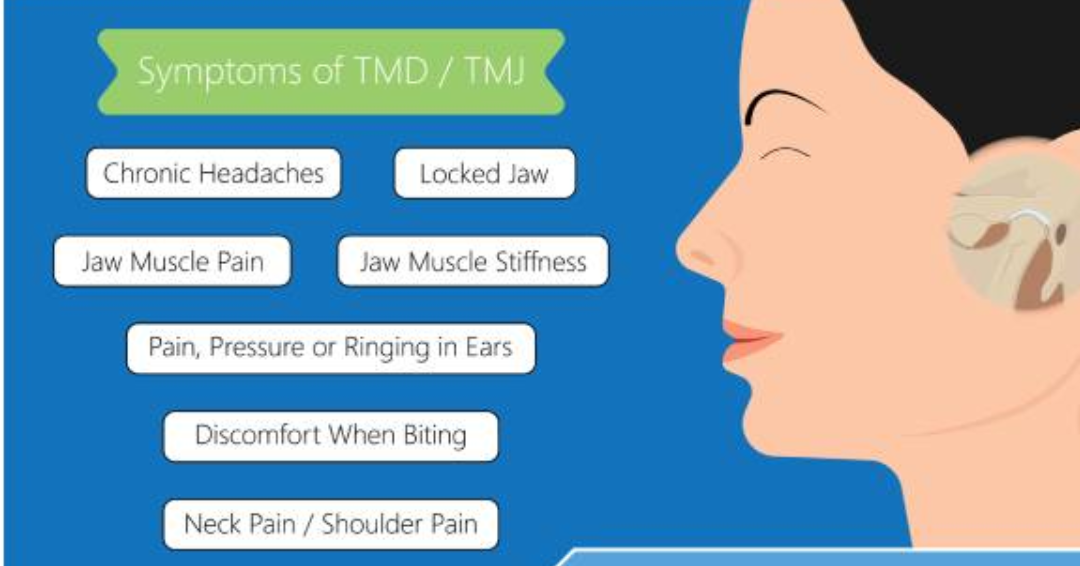
As a chiropractor, I have strong interest in musculoskeletal conditions and obviously most of our patients come to meet us because of them.
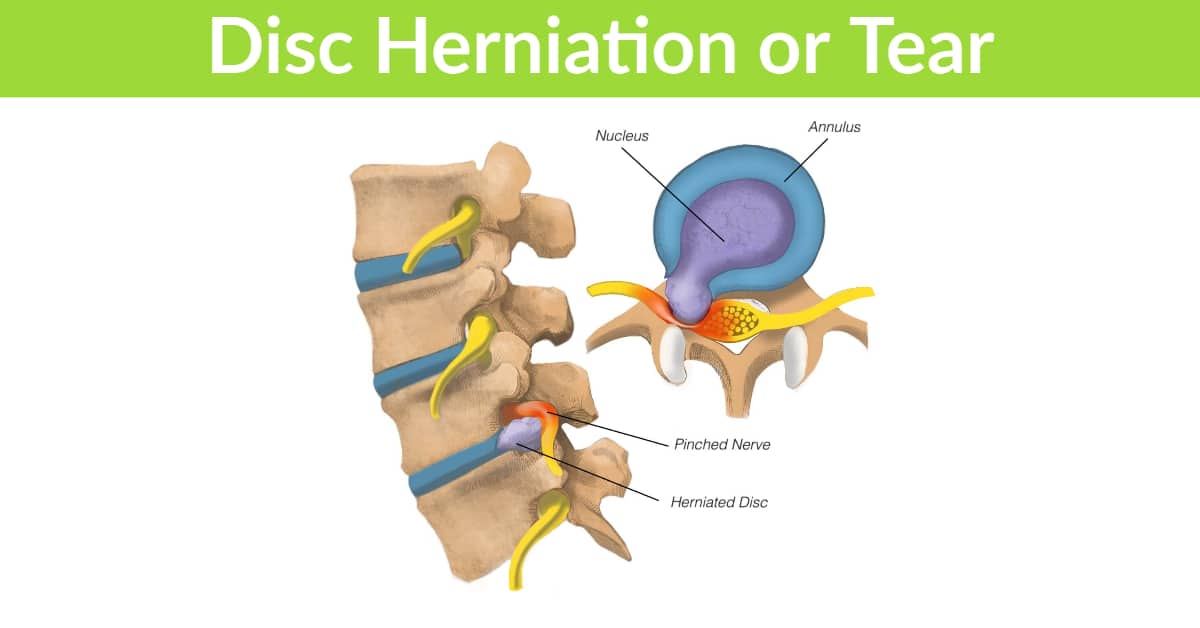
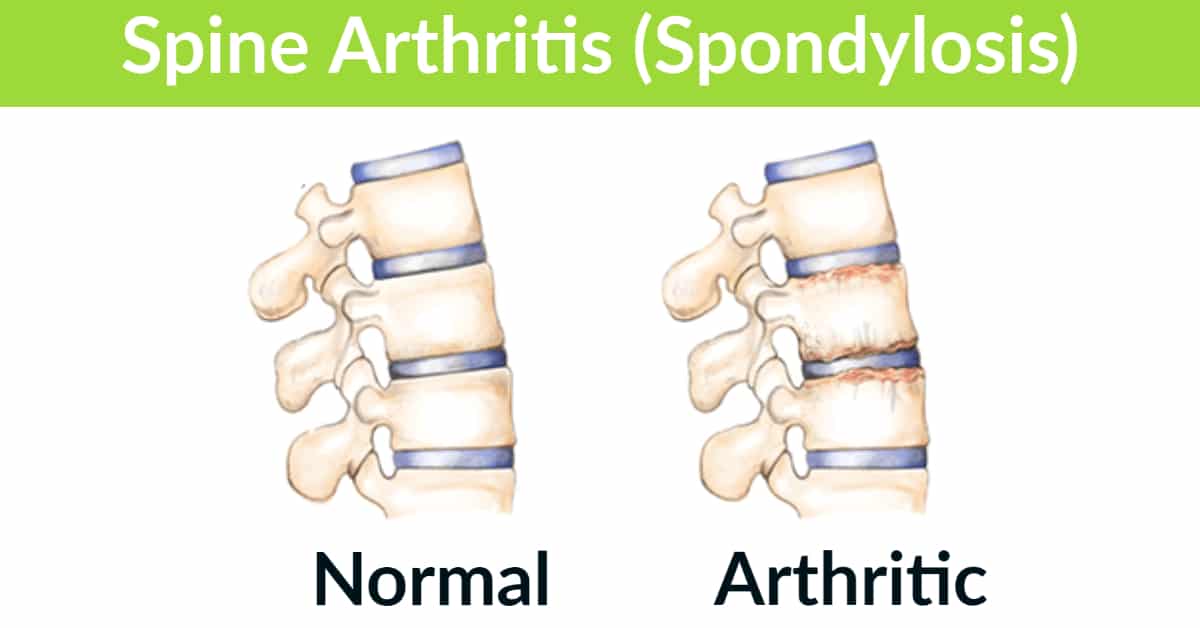
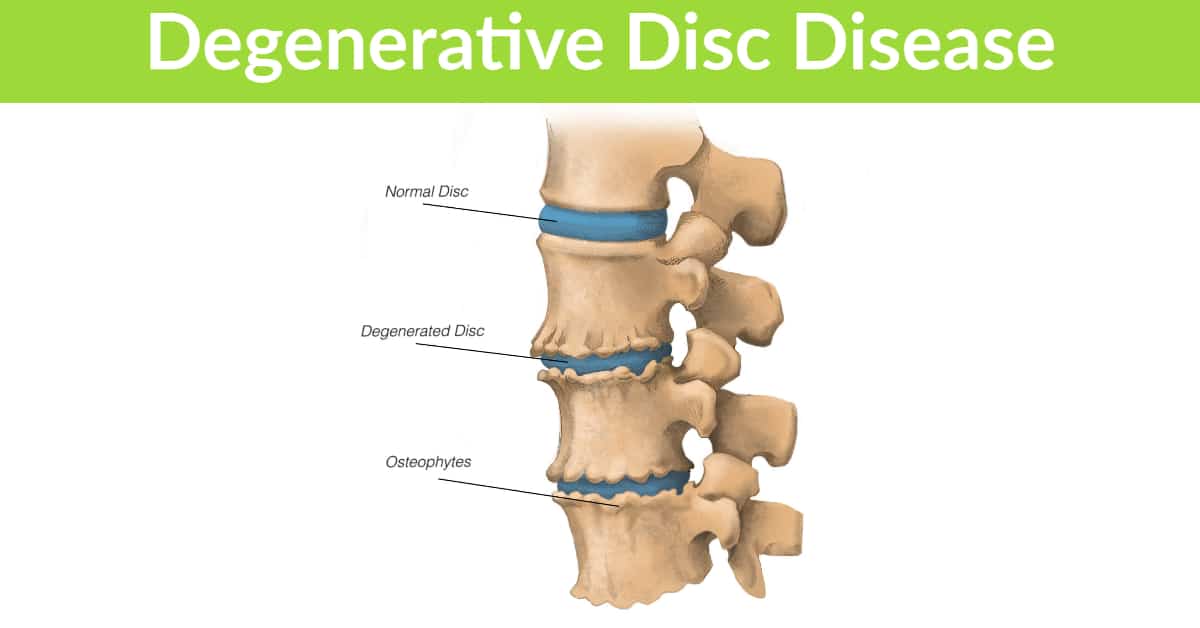
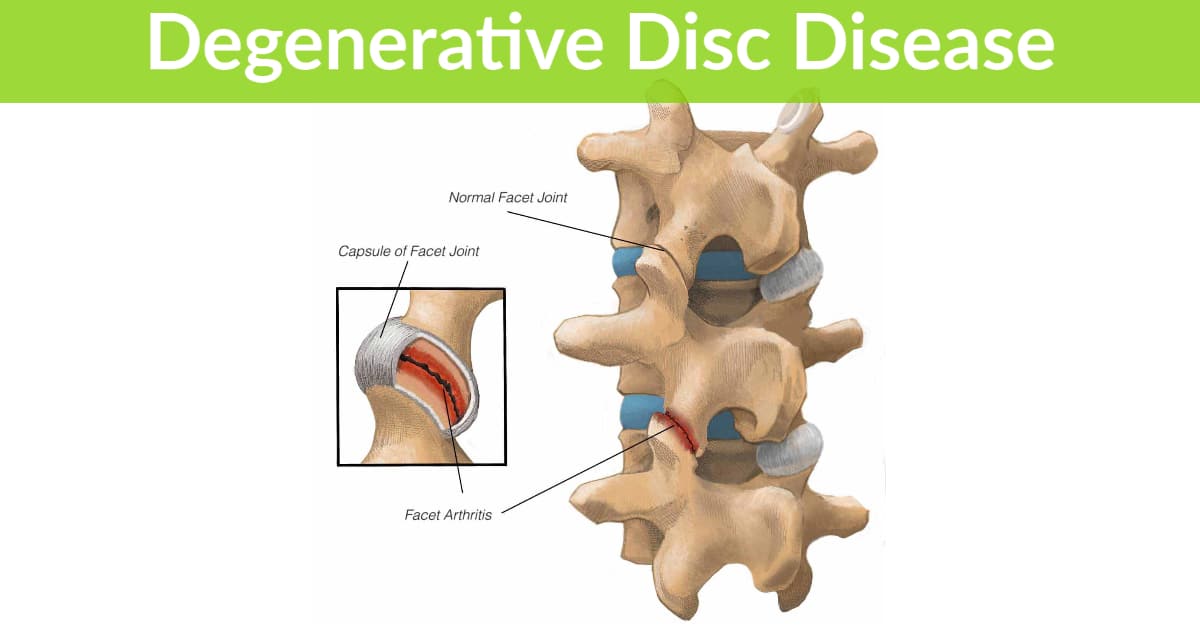
Successful treatment of joint pain, arthritis and degeneration, muscle injuries (strains, torn muscles), tendonitis, ligament damage or sprains all involve a combination of both passive and active treatments.
Active treatment consists of corrective and therapeutic exercise, posture awareness, biomechanical correction, strength training, etc. Basically this means you have to do the work to get the results.
Passive treatment consists of manual therapy and massage, dry needling and trigger point therapy, steroid or cortisone injections and pain medication. All passive treatments are obviously easier to get done, but not as effective as active therapies in the long run.
In this article, I want to share some exciting news about a passive therapy called Shock Wave Therapy (Extracorporeal Shock Wave Therapy) that has many advantages including:
- It works.
- It's non-invasive (no risk of infection or needles required)
- No risk of tissue damage (like you get from steroid injections)
- FDA cleared and approved for multiple conditions
- Extensively backed by basic science and clinical science research
What Is Shock Wave Therapy?
Shock Wave Therapy, or Extracorporeal Shock Wave Therapy (EWST), is a non-invasive treatment that involves the delivery of shock waves to an injured area to promote healing.
This treatment produces highly effective shock waves that initiate biological regeneration processes at the cellular level.
The treatment involves applying short, frequent, and high intensity bursts of mechanical energy (in the form of a shockwave) into injured soft-tissue, scarred soft tissue, or tissue that is painful, inflamed and contains adhesions.
There are now 3400 scientific papers describing the cellular and biological mechanisms behind shock wave therapy. [1]
Shock Wave Therapy causes three specific responses to the tissue including:
- Physical Response – shock waves hit the tissue and generate positive pressure waves
- Chemical Response – the pressure waves mechanically stimulate biochemical reactions that cause our cells to become activated
- Biological Response – the cells receive instructions to stimulate remodeling of blood vessels, reduction of inflammation molecules and the stimulation of new and healthy tissue (muscles, ligaments and tendons)
All together, the scientific knowledge of shock wave therapy can be summarized by the following graphic:
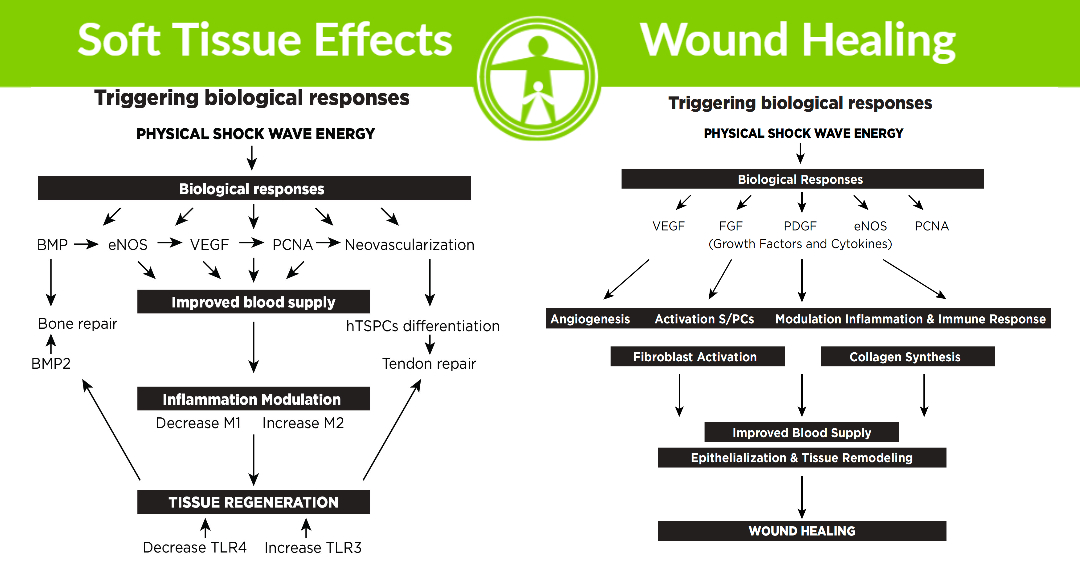
What are the Therapeutic Effects of Shock Wave Therapy?
Shock waves have the ability to grow new blood vessels and activate the production of healthy connective tissue. They help to relieve pain and heal painful joints and areas in the spine with zero needles.
Shock wave therapy was originally known as a treatment of tendinopathies and muscle damage, but recent research has demonstrated success in areas of regenerative medicine like spinal cord injuries and vascular & nerve regeneration.
Shock waves have specific therapeutic effects including:
- Pain relief – analgesic effect
- Anti-inflammatory action:
- Lowers the pro-inflammatory immune response
- Decreases cellular apoptosis and reduces necrosis (programmed cell death)
- Antibacterial effect in the treatment of infections
- Induces the expression of endogenous growth factors (stimulates tissue regeneration)
- Angiogenesis; improved vascularity and blood circulation, tissue supply
- Ossification; formation of new bone tissue
- Stimulates natural anabolic and growth functions in all kinds of tissues
(skin, bones, cartilage, smooth & striated muscles, nerves…) - Activation of stem cells; metabolism ↑, proliferation ↑, migration ↑, differentiation ↑
- Tissue remodeling and regeneration
Taking into account all the above, extracorporeal shockwave therapy (SWT) can be used for the treatment of a variety of musculoskeletal conditions, primarily applied to chronic conditions, particularly those affecting medium to large sized tendons and their insertions on bone such as:
- Upper and Lower extremity tendinopathies
- Plantar Fasciitis
- Achilles Tendinopathy
- Retrocalcaneal Bursitis
- Lateral Epicondylitis (Tennis Elbow)
- Medial Epicondylitis (Golfer’s Elbow)
- Calcific Tendonitis (supraspinatus tendon, etc.)
- Patellar Tendinosis (Jumper’s Knee)
- Morton’s Neuroma
- Chronic Stress/Non-union Fractures

What Can You Expect with Shock Wave Therapy?
The procedure averages 10-15 minutes but may be longer depending on treatment area and diagnosis. A gel (typically ultrasound gel) is applied to the surface area to be treated. The applicator produces pulses as the clinician moves around the treatment area.
During therapy, communication with the provider is necessary to identify treatment areas and monitor progress. Shockwave, like many medical procedures is probably best described as uncomfortable.
Of course is very subjective, person to person.
A few key features of treatments include:
- Non-invasive
- No anesthesia or numbing creams needed
- No side effects
- Same day procedure
- Long lasting
Shockwave is unsuitable in the following circumstances:
- If you are pregnant
- If you have a blood clotting disorder (including thrombosis)
- If you are taking oral anti-coagulants
- If you have received a Steroid injection within 6 weeks
- If you have a Pacemaker fitted
- if tumors are present at the treatment site
- if you have an infection or skin abrasion at the treatment site
- if you are Under 18 (except in the treatment of Osgood-Schlatter disease).

Next Steps
Most people think the only option to deal with ongoing tendon or joint pain is surgery or living with the symptoms. The good news is, there is an alternative and Shockwave therapy may be a solution to helping your body overcome long lasting, nagging injuries.
If you're interested in obtaining Shock Wave Therapy at our office, call 512-347-8881 or contact us online to learn more.